
In the early days of the COVID-19 pandemic, many people first learned about a small medical device called a pulse oximeter. The device clips onto the fingertip and within seconds, measures the oxygen level in a person’s blood. Pulse oximeters grew in popularity during the pandemic as more people became interested in monitoring themselves for a drop in oxygen levels, a symptom of COVID-19 that warrants immediate medical attention.
Jesse Jokerst, a professor of nanoengineering at the University of California San Diego, also keeps a pulse oximeter on hand in his lab, but for a different reason. His interest in the device stems from a particular problem that runs skin-deep: pulse oximeters can be less accurate on darker skin tones.
Recent studies have shown that oximetry tests performed on patients with darker skin tones—specifically Asian, Black and Hispanic patients—typically produce falsely high blood oxygen measurements. As a result, these patients often receive less supplemental oxygen than white patients who have similar true blood oxygen levels. Supplemental oxygen is critical for treating heart and lung conditions characterized by low blood oxygen levels, such as congenital heart disease, pulmonary edema and chronic obstructive pulmonary disease. More studies are revealing that failure to administer supplemental oxygen, or completely missing these diagnoses due to inaccurate blood oxygen readings, is contributing to the existing racial inequities in health care.
These inaccuracies arise because of how pulse oximeters rely on light to measure oxygen levels. The device shines a beam of light through the skin and into the bloodstream. The amount of light that is reflected to the device is correlated to a person’s blood oxygen level. More light detected means a higher blood oxygen level at that location. But if something gets in the way of that light—like melanin, a pigment in the skin—it can decrease the accuracy of the measurement. Melanin affects the reading in two ways: it blocks some light from penetrating into deeper tissues and at the same time, it reflects that light back to the device.
It’s like trying to see a person’s eyes while they are wearing reflective sunglasses, explained Jokerst. It’s difficult because the sunglasses are protecting the person’s eyes by reflecting the incoming light and not letting as much of it shine through.
“Now imagine your skin now is like those sunglasses,” said Jokerst. “The darker the skin tone, the more melanin there is to block out and reflect light, like an additional pair of sunglasses More and more of the light from the oximeter is going to get filtered out and bounced back. That results in a less accurate reading.”
As a result, darker skin tones lead to overreported blood oxygen measurements at the surface of the skin.
The discrepancy between skin tone and accuracy of blood oxygen readings, noted Jokerst, is a physical limitation of how light interacts with pigment in the skin. This limitation motivated Jokerst, an expert in optical imaging, to engineer a solution.
Jokerst is among a growing number of scientists who are tackling the skin tone issue in blood oxygen measurements. Various research groups are focused on fixing the issue in pulse oximeters, but Jokerst is taking a slightly different approach. In this case, he is focused on fixing the issue in a type of oximetry called photoacoustic oximetry.
Photoacoustic oximetry vs. pulse oximetry
Photoacoustic oximetry is emerging as an alternative to pulse oximetry. It is currently used in clinical settings as well as preclinical research to measure blood oxygen levels. It is similar to pulse oximetry in that it sends a beam of light through the skin to measure oxygen content or image features beneath the skin. But instead of detecting the amount of light reflected back like in pulse oximetry, photoacoustic oximetry detects the sound waves emitted by the tissue. This produces a spatial image, or map, of oxygen concentration in the blood, instead of a single numerical reading as in pulse oximetry.
This makes photoacoustic oximetry a more powerful method because it can provide entire images of deeper tissues and spatial maps of blood oxygen content in any part of the body. Physicians and researchers can use it to get a more accurate measure of blood oxygen levels in specific areas, such as near wounds or at the heart. Meanwhile, pulse oximetry is limited because it only measures oxygen concentration at the sites it is placed, usually the fingertip, toe, or ear.
Despite its advantages, photoacoustic oximetry is plagued by the same skin-deep problem as pulse oximetry: it can overreport oxygen levels at the surface of the skin in individuals with darker skin tones. Moreover, it can also underreport blood oxygen readings in tissues deep beneath the skin in these same individuals. This is because it still relies on sending light through the skin. Melanin in the skin’s upper layers reflects light from the oximeter and prevents it from reaching deeper tissues. Since so much light is reflected at the surface of the skin, less light can penetrate into deeper blood vessels or tissues, which means fewer sound waves are emitted by the tissue. This in turn makes it difficult to take high resolution images of blood oxygen content in these parts of the body and leads to underreported oxygen levels in deeper blood vessels or tissue.
A step to improving equity in health care
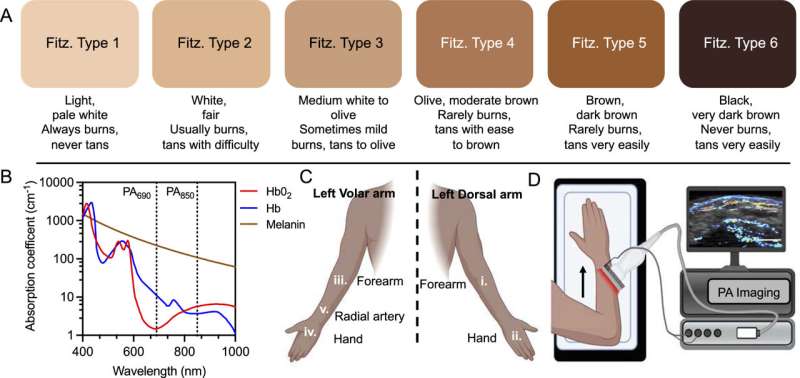
Jokerst’s lead student on the project, Yash Mantri, who recently earned his Ph.D. in nanoengineering at UC San Diego, observed this discrepancy firsthand while working on this project. He recruited 9 healthy subjects with a range of skin tones and imaged the radial artery on their forearms using a photoacoustic oximeter in the lab. He found that the oxygen signals were both much lower in deeper blood vessels and higher at the skin surface in subjects with darker skin tones than in subjects with lighter skin tones.
Jokerst and Mantri saw an opportunity to help eliminate this discrepancy and make biomedical imaging more equitable. “We see photoacoustic oximetry as a broadly applicable technology, and we’re trying to make sure everyone benefits, not just one subset of patients,” said Jokerst.
The team developed an equation to correct for differences in skin tone. First, the researchers compared blood oxygen readings from photoacoustic oximetry and pulse oximetry measurement. They used that data to correct the artificially low oxygen levels detected in deeper blood vessels of individuals with darker skin tones. The researchers then established linear correlations between darker skin tones with lower blood oxygen levels in deeper blood vessels. The resulting equation was able to produce an increased—and more accurate—measure of blood oxygen levels for individuals with darker skin tones.
To validate the equation, Mantri measured the oxygen level in the radial artery in two additional participants with skin tones in between the original 9 subjects and applied the correction factors. This method accounted for the lower oxygen signal in photoacoustic oximetry readings with a less than 3% error compared to pulse oximetry. The simple equation to adjust the photoacoustic oximetry readings was accurate with the new subjects and could be extended to other skin tones. The researchers published their findings in the journal Biomedical Optics Express.
Jokerst and Mantri hope that their work will inspire other engineers to consider skin tone when developing new medical devices and techniques. In order to design devices with equitable outcomes in health care, differences in skin tone in patients must be considered during—not after—development, they noted in their paper.
Source: Read Full Article