
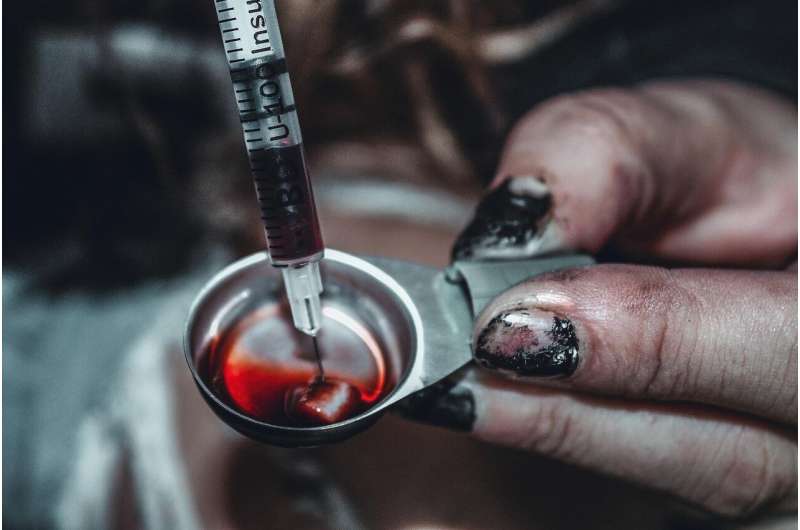
For people at high risk of overdose enrolled in a safer opioid supply (SOS) program, there was a rapid decrease in emergency department visits and hospitalizations soon after initiation, according to new research published in Canadian Medical Association Journal (CMJA). These programs may help to address the devastating drug poisoning overdose crisis in Canada.
The opioid overdose crisis is a major public health concern, with more than 29 000 opioid-related deaths occurring in Canada from 2016 through 2021, driven mainly by drug poisoning from high and unpredictable levels of fentanyl in the unregulated drug supply. The COVID-19 pandemic has worsened the overdose crisis, and safer supply programs have been proposed as one potential intervention that may help to address the crisis.
Safer opioid supply programs work to reduce harms by providing prescription opioids to people at high risk of overdose as an alternative to using fentanyl from the unregulated drug supply. Immediate-release hydromorphone is most often prescribed—dispensed daily and provided as take-home doses. Some programs also provide additional health and social supports, such as comprehensive primary care, treatment for medical conditions and access to social support workers.
However, published evidence on the real-world impacts of SOS programs is lacking.
To understand the impact of one such program, researchers looked at health outcomes, health services utilization and health care costs associated with the introduction Canada’s first formal SOS program, started at the London InterCommunity Health Centre (LIHC) in London, Ontario, in 2016. They looked at data from 82 clients in the program to see how their health outcomes changed after starting the program and compared their outcomes to those of local residents diagnosed with an opioid use disorder who were not exposed to the program. Among program participants, the researchers saw a rapid decrease in emergency department visits, hospitalizations (including hospitalizations for certain bacterial infections associated with injection drug use) and health care costs (excluding costs related to primary care and medication) after the program began.
“These positive impacts were seen very quickly after entering the program,” said lead author Dr. Tara Gomes, Unity Health Toronto and ICES, Toronto, Ontario. “We did not see similar changes in a matched group of people with opioid use disorder not enrolled in the program, suggesting that these changes seen in safer supply clients were because of participation in the program, and were not influenced by outside factors.”
The average age of people in the study was 41 years and 40% were male. High rates of HIV (34%), Hepatitis C (69.5%) and infectious complications (28%) in the year before enrolment suggests the program is reaching a group of people who had been experiencing serious medical complications from drug use.
No opioid-related deaths occurred among the SOS participants during the 6-year study period.
“There have been concerns raised about SOS programs, and both the improvements in health services usage and lack of negative outcomes detected among clients provides important reassurance about the safety of these programs,” said Dr. Gillian Kolla, Canadian Institute for Substance Use Research, University of Victoria, Victoria, British Columbia. “It is important to note that the London program also offers comprehensive primary care and social supports to safer supply clients, so it will be important for future research to examine the impact of different program elements on client outcomes.”
The authors note that more research is needed to understand the benefits and potential risks of SOS programs, but this initial work suggests positive benefits to participants.
Source: Read Full Article