
A new test to detect womb cancer could prevent 87% of women who do not have cancer from needing invasive diagnostic procedures, finds a new study led by researchers at UCL and the University of Innsbruck.
The test, called WID-qEC, could simplify and speed up the pathway to a diagnosis of womb cancer or ruling the condition out as a cause of symptoms.
The research, published in The Lancet Oncology, shows that the WID-qEC test outperforms imaging at ruling out womb cancer and could save nearly 90% of peri- and post-menopausal women from needing invasive surgical biopsies when getting abnormal vaginal bleeding symptoms checked.
This could save thousands of women each year from potentially painful surgical biopsies and increased anxiety while waiting for answers.
Professor Martin Widschwendter (UCL EGA Institute for Women’s Health and University of Innsbruck), said, “One of the most important principles of modern preventative medicine is ‘less is more.’
“The WID-qEC test is an ideal example of this. It significantly reduces the complexity of the pathway which women, presenting with abnormal bleeding, currently have to undergo.
“We’re excited that the test will be commercially available in Austria and Switzerland from early 2024 and are actively working toward commercialization in other countries including the U.K. in the coming months.”
Womb cancer is the fourth most common cancer in women in the U.K. However, it can be difficult to detect, as the main symptom—abnormal vaginal bleeding—can also be caused by multiple non-cancerous conditions that are difficult to distinguish from cancer with imaging alone.
For example, approximately 800,000 women and people with gynae organs report abnormal bleeding in the U.K. and nearly 11,400 each year will go on to be diagnosed with womb cancer.
Current procedure in the U.K. is for patients presenting with abnormal vaginal bleeding to be offered either a transvaginal ultrasound (where a scanner probe is inserted into the vagina to visualize the inside of the womb) or other techniques to look for a thickened womb lining (endometrium).
As a thickened womb lining can be caused by many things, most of which are non-cancer related, a biopsy is needed to diagnose the cause.
In most cases women require a surgical procedure to collect the biopsy. This will involve a hysteroscopy (a narrow telescope with a light and small camera at the end, which is placed into the vagina, passed through the cervix and into the womb) followed by a biopsy. These procedures are invasive and often painful.
The WID-qEC would enable women going to the doctor to discuss abnormal vaginal bleeding to have a sample taken from the vagina during their appointment to send off for testing. The sample would be tested using PCR, which is relatively low-cost and is already routinely used, for example in the detection of coronavirus.
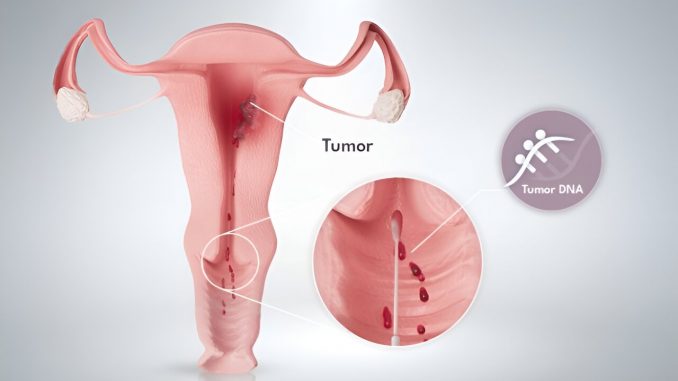
The test looks at “tags” on the top of the DNA called DNA methylation. DNA from cancer cells has a particular pattern of DNA methylation, like a unique barcode that can be specifically “scanned” by the WID-qEC test, to tell if there is womb cancer present, or not.
If someone’s test came back as positive for a potential cancer, they would then need a biopsy to confirm their diagnosis.
The clinical trial involved 400 peri- and post-menopausal women with abnormal vaginal bleeding who were being investigated at the UCLH gynecological rapid access clinic, which is a center of excellence.
A sample was taken for the WID-qEC test before their initial ultrasound scan, and they then continued down the current pathway for womb cancer investigation. Twelve of the women had womb cancer.
In total, 603 imaging tests were done (transvaginal, transrectal or transabdominal ultrasounds, saline infusion sonography or MRI), with nearly 40% of patients needing more than one imaging test to decide their next steps. Endometrial thickness measurements from imaging required follow up with a surgical diagnostic procedure in 75 women without cancer. In contrast, only 10 women without cancer had a positive WID-qEC test result that would have required follow up with a surgical diagnostic procedure.
The results found that both ultrasound imaging and the WID-qEC, picked up 91% of womb cancer cases—highlighting how the new technique could simplify and speed up the route to rule out or diagnose womb cancer, enabling people to start treatment sooner while saving time and money.
Athena Lamnisos, CEO, The Eve Appeal, said, “We hear from many women who have been investigated for abnormal bleeding, and they have really varied experiences of hysteroscopy and biopsies, some manage this procedure fine, but for many it is extremely painful.
“On top of this, the waiting time between thinking you may have a potential cancer and finding out your results is agonizing. Saving thousands of women from needing to go through the pain of tests and speeding up the wait before cancer being ruled out or diagnosed and starting treatment is very welcome progress.”
More information:
Iona Evans et al, Performance of the WID-qEC test versus sonography to detect uterine cancers in women with abnormal uterine bleeding (EPI-SURE): a prospective, consecutive observational cohort study in the UK, The Lancet Oncology (2023). DOI: 10.1016/S1470-2045(23)00466-7
Journal information:
Lancet Oncology
Source: Read Full Article