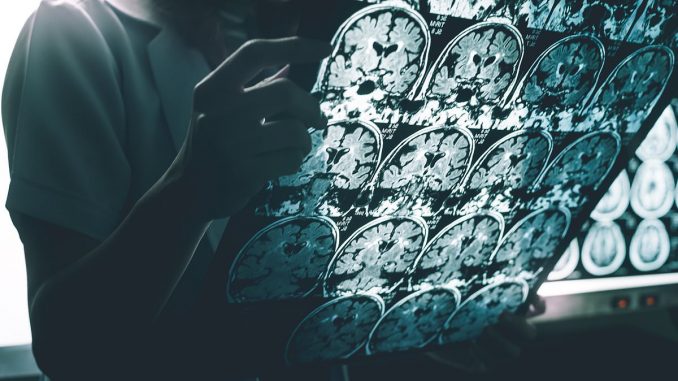
Woman who has one in 7bn genes that make her ‘IMMUNE to Alzheimer’s’ may offer clues to beat disease
- The Colombian woman has two copies of a rare variant of the APOE gene
- This is called the Christchurch mutation, and could hold the key to therapies
- READ MORE: Multiple sclerosis medication may potentially treat Alzheimer’s
A woman who has avoided Alzheimer’s despite the disease blighting most of her family may offer clues as to how to beat it, a study suggests.
The unnamed Colombian woman, now in her late 70s, has kept fit and healthy despite half of her family coming down with the condition and some even developing it in their 40s.
She carries two copies of a rare variant of the APOE gene, called the Christchurch mutation, and is the only person in the world known to do so.
In the latest study, researchers at Washington University in St Louis used genetically altered mice to show that the mutation cuts the link between the early phase of Alzheimer’s, when amyloid beta collects in the brain, and the later stage, when tau tangles build up and cognitive decline starts.
Alzheimer’s disease causes around two thirds of cases of dementia and is triggered by the build-up of protein clumps called plaques, which interrupt and destroy nerve cells in the brain and prevent it from functioning normally
They found that with the mutation, the brain’s waste disposal cells were more efficient at getting rid of tau tangles.They found that with the mutation, the brain’s waste disposal cells were more efficient at getting rid of tau tangles.
This means the woman’s brain was still filled with amyloid, but she remained mentally sharp.
Dr David Holtzman, lead author of the study and professor of neurology, said: ‘Any protective factor is very interesting, because it gives us new clues to how the disease works.
WHO ARE THE COLOMBIAN FAMILY PLAGUED BY EARLY-ONSET ALZHEIMER’S?
An extended family consisting of around 6,000 members, who live in and around the Colombian city of Medellín in the country’s Antioquia region, are known to have an inherited form of Alzheimer’s disease.
Scientists have found that, for decades, most members of the community have developed Alzheimer’s disease in their 40s and 50s.
Typically, the brain-destroying disease does not begin until someone is much older.
The family, whose family tree stretches back some 300 years, have been found to have a genetic mutation which is responsible for the disease.
The mutation is on a gene called presenilin 1 (PSEN1).
PSEN1 is responsible for the creation of the amyloid protein which builds up to create toxic, brain-damaging clumps on the nerve cells of Alzheimer’s patients.
Mutations make it more likely that damaging amounts of the protein will be created, and are one of the main reasons for familial Alzheimer’s disease.
Some people in the Colombian family with the PSEN1 mutation were observed to develop Alzheimer’s slightly later than others, lasting into late middle age, but none have yet been found to escape it completely.
Sources: Nature; Stat
‘As people get older, many begin to develop some amyloid accumulation in their brains.
‘Initially, they remain cognitively normal. However, after many years the amyloid deposition begins to lead to the accumulation of the tau protein.
‘When this happens, cognitive impairment soon ensues. If we can find a way to mimic the effects of the APOE Christchurch mutation, we may be able to stop people who already are on the path to Alzheimer’s dementia from continuing down that path.’
This may lead to the creation of new drugs which imitate the impact of the mutation and stop amyloid in people’s brains deteriorating into Alzheimer’s.
Alzheimer’s builds up over roughly 30 years, with the first two decades happening silently as amyloid gathers but no negative effects are caused.
When the amount of amyloid reaches a tipping point, tau tangles will spread through the brain, causing cell death.
The brain will slow down and begin to shrink, leading to thinking and memory issues.
Dr Holtzman said: ‘One of the biggest unanswered questions in the Alzheimer’s field is why amyloid accumulation leads to tau pathology.
‘This woman was very, very unusual in that she had amyloid pathology but not much tau pathology and only very mild cognitive symptoms that came on late. This suggested to us that she might hold clues to this link between amyloid and tau.’
The researchers used mice genetically modified to overproduce amyloid and altered them to carry the human APOE gene with the Christchurch mutation.
Then they injected the mice’s brains with a small amount of human tau, which would usually see tau spread throughout the brain.
However, similarly to the Colombian woman, the mice only developed minor tau spreading, despite having lots of amyloid.
The researchers realized the vital difference was how active the brain’s waste disposal cells were, called microglia.
In the mice with the APOE Christchurch mutation, the microglia surrounding amyloid plaques were very efficient at getting rid of tau clusters.
Dr Holtzman said: ‘These microglia are taking up the tau and degrading it before tau pathology can spread effectively to the next cell.’
‘That blocked much of the downstream process; without tau pathology, you don’t get neurodegeneration, atrophy and cognitive problems.
‘If we can mimic the effect that the mutation is having, we may be able to render amyloid accumulation harmless, or at least much less harmful, and protect people from developing cognitive impairments.’
The study was published in the journal Cell.
Source: Read Full Article